Clocks go forward Dementia Tips

For the majority of people, changing the clocks can be a minor nuisance, but for people living with dementia it can be disorientating and sometimes cause anxiety and distress.
As daylight begins to start earlier and end later, people with dementia may find it difficult to differentiate between 6am and 6pm. This can disrupt their circadian biological clock and make it hard for them and those who care for them to get enough sleep. The Alzheimers Society has 4 great tips.
Alzheimers Society 4 great tips
Prepare on Saturday evening
Think about having dinner and going to bed an hour earlier on Saturday, so that the person can still get their usual amount of sleep and wake up at their usual time on Sunday. In this way, the person’s routine will only be different for an evening rather than a full day.
Routine
Having a routine during the day and at bedtime can help regulate a person’s disrupted body clock. Doing regular activities at the same time each day – for example, going for a walk after breakfast can help a person with dementia make sense of the time.
Outside time
Going outside and getting some gentle exercise can help the person feel sleepier during the evening so they go to bed at their usual time.
If the person is unable to go outside, helping them keep active during the day can have a similar effect. Think about using blackout curtains to reduce sunlight in the evenings too.
Auto setting clocks
www.alzheimers.org.uk
Carers UK supports “Share for Better Care”

Carers UK is supporting the Care Quality Commission’s (CQC) Share for Better Care campaign by encouraging unpaid carers across England to speak up about their experiences of health and social care.
The campaign, run in partnership with Healthwatch England, aims to ensure that the voices of people who use care services are heard and used to improve services. It particularly seeks feedback from people whose voices may be under-represented
More Information
Carers UK is promoting the campaign, which takes place from 23rd-29th March 2026, and is encouraging carers to take part by sharing their feedback on services they and the people they care for rely on. Insights gathered through the campaign help inform how services are monitored and improved across England.
Unpaid carers have an important insight into how care works day to day – from leaving hospital to getting support at home. They are often the ones spotting gaps, chasing support and helping services work together. By sharing their experiences, carers can help make care more joined-up, responsive, and better for everyone.
Emily Holzhausen CBE, Director of Policy and Public Affairs at Carers UK, said:
“Unpaid carers know what works and what doesn’t in health and social care. Their experiences give a unique insight into the challenges and gaps in services. Over half (53%) of carers say they feel angry and frustrated about their situation, often due to a lack of support from health and social care services. We want to encourage carers to share their experiences so that services can learn, improve and better support families.”
2026 Travelling abroad

New border systems and rule changes come into force this year. Find out how they’ll affect you if you’re travelling abroad. Ageco offer great advice on new rules.
If you’ve travelled abroad in 2026 you might notice things feel a little different. More and more countries are requiring new digital procedures with added steps when crossing borders. Once you have your travel insurance in place, here are some things to watch for when heading off on your holidays.
More Information
If Europe is on your list this year, you’ll find the biggest travel rule changes at the border. By 10th April, the EU’s new EES will have been rolled out at all external Schengen area borders (this is the area of European countries with freedom of movement between them and encompasses most of the European continent) replacing manual passport stamping with a digital record of arrivals and departures.
Your photo and fingerprints may be taken the first time you enter. The European Commission has indicated that these checks might be eased during busy periods, but make sure to build in extra time for queuing.
Some pensioners to get £100 to buy food and fuel

A council is offering up to £100 to some pensioners to help them buy food and fuel.
Preston City Council’s new scheme is open to those who get council tax support but are not in receipt of pension credit.
The authority said it was limited to £100 per household to help with the “rising prices for food, utilities, and housing”. Residents can apply.
Apply here
12 Ways to Prevent Falls

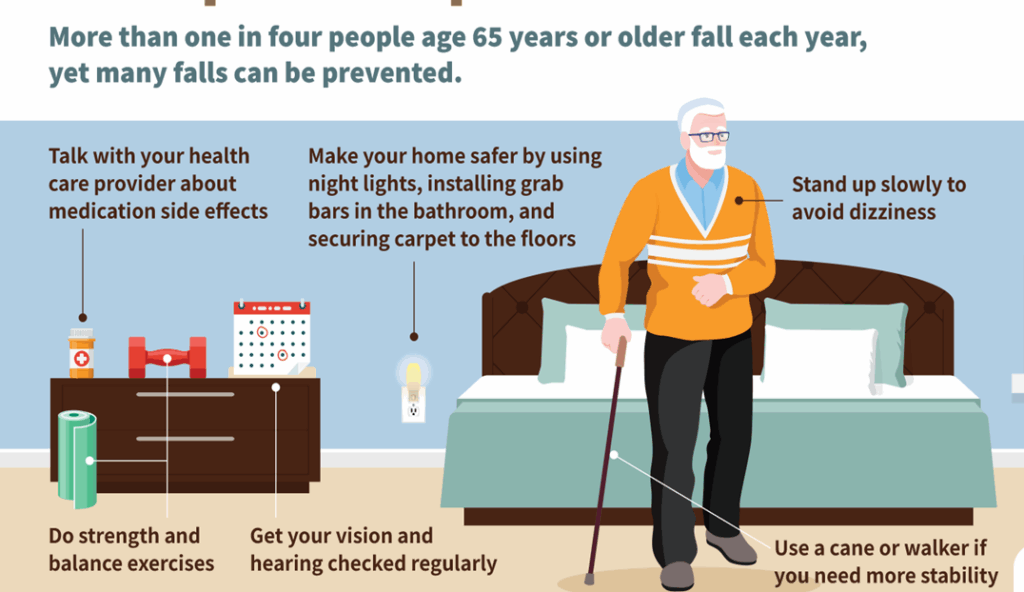
Nearly a third of people aged 65 and over will fall at least once a year, and as age increases, so does the risk, with around half of the over-80s taking a tumble.
Around 255,000 older people are admitted to hospitals in England every year after falling, and even if bones aren’t broken (most falls don’t result in serious injury), falls destroy confidence, increase isolation and reduce independence
12 Ways to help Prevent Falls
- Be aware of who’s most at risk – older people are more likely to fall because they have balance problems and muscle weakness, poor vision, or a long-term health condition such as heart disease, dementia or low blood pressure.
- Book a medication review every six months with your GP or pharmacist, as some medications can increase the risk of falls due to side-effects.
- Make sure there are bannisters or handrails where needed.
- Buy shoes and slippers with a good fastening and support and a sturdy sole.
- Improve strength and balance by joining local exercise classes or doing other activities – a tailored exercise programme can reduce the risk of falling by up to 50%.
- Use non-slip mats in the bathroom, and consider having a shower seat.
- Mop up spills to prevent slippery floors.
- Get help lifting or moving items that are heavy or difficult to lift.
- Remove clutter.
- Ensure all areas of the home are well lit.
- Have a sight test – It’s estimated that around 30% of visual impairment in people over 75 is the result of wearing the wrong glasses or no glasses at all, which can affect balance and coordination.
- Your GP may recommend you have an electrocardiogram (ECG) and have your blood pressure checked.
What to do if You Fall
The risk of falling increases with age. Falls can be especially dangerous for older adults, often causing fractures, hospitalization, and disability.
The good news is that many falls are avoidable. But what if you do fall. Some common sense tips if you take a tumble
What to do if you Fall
- Keep calm.
- If you’re not hurt, don’t get up quickly. Roll onto your hands and knees and hold on to a stable piece of furniture with both hands. Slowly get up, and then sit down and rest.
- If you’re hurt or unable to get up, try to get someone’s attention by calling for help, banging on the wall or floor, or using an call aid button, If possible, crawl to a telephone and dial 999 for an ambulance.
4. Try to reach something warm to put over you, such as a blanket or dressing gown
Endangered Homes over 2 million

The Centre for Ageing Better and Care & Repair England’s new report reveals that over two million over-55s are living in a home that endangers their health or wellbeing.
The report into non-decent housing in England found that over 4.3 million homes in England don’t meet basic standards of decency, most commonly because of the presence of a serious hazard to their occupants’ health or safety.
More Information
Poor housing can cause or worsen health conditions, reduce a person’s quality of life, exacerbate inequalities and can even result in premature death. Despite this evidence, an estimated 10 million people in England are at risk because they live in a poor-quality home. This is the equivalent of 4.3 million homes, close to half of which are homes lived in by someone over 55 years old and a million with at least one child.
This report uses both previously published and new analysis by the Building Research Establishment (BRE) of the latest English Housing Survey (EHS) data (collected in 2017 and published in 2019). The aim of this report is to provide an overview of housing conditions in England, particularly in the context of population ageing, to inform the policy and practice that relates to ageing well at home.
Beware of the Heat

Too much heat is not safe for anyone. It is even riskier if you are older or have health problems. It is important to be cautious and get relief quickly when you are overheated. Otherwise, you might start to feel sick or risk a heat-related illness that could cause serious health issues.
Why can extreme weather be even more dangerous for older adults than for younger people?
Heat problems to be aware of
Hotter days can cause difficulty in the body’s ability to regulate its temperature. This can be challenging for older adults who typically do not adjust as well as others to sudden temperature changes. Additionally, older adults are more likely to have chronic medical conditions that affect the body’s response to temperature, and to take prescription medicines that alter the body’s ability to control temperature or sweat. Typical heat problems:
- Heat syncope is a sudden dizziness that can happen when you are active in hot weather. If you take a heart medication called a beta blocker or are not acclimated to hot weather, you are even more likely to feel faint. Rest in a cool place, put your legs up, and drink plenty of water to make the dizzy feeling go away.
- Heat cramps are the painful tightening or spasms of muscles in your stomach, arms, or legs. Cramps can result from hard work or intense exercise. Though your body temperature and pulse usually stay normal during heat cramps, your skin may feel moist and cool. Stop the physical activity you’re doing and rest in the shade or in a cool building. Drink plenty of fluids, such as water and sports drinks containing electrolytes. Do not consume alcohol or caffeinated beverages.
- Heat edema is a swelling in your ankles and feet when you get hot. Put your legs up to help reduce swelling. If that doesn’t work fairly quickly, Consult your Doctor.
- Heat rash is a skin irritation from heavy sweating. It causes red clusters of small blisters that look similar to pimples on the skin. Your skin may feel itchy or you may feel “prickly” tingling pain. Keep the infected area dry, use powder to sooth the rash, and stay in cool areas.
- Heat exhaustion is a warning that your body can no longer keep itself cool. You might feel thirsty, dizzy, weak, uncoordinated, and nauseated. You may sweat a lot. Your body temperature may stay normal, but your skin may feel cold and clammy. Some people with heat exhaustion have a rapid pulse. Rest in a cool place and get plenty of fluids. If you don’t feel better soon, get medical care. Be cautious because heat exhaustion can progress to heat stroke.
- Heat stroke is a medical emergency in which the body’s temperature rises above 104°F. Signs of heat stroke are fainting; confusion or acting strangely; not sweating even when it’s hot; dry, flushed skin; strong, rapid pulse; or a slow, weak pulse. When a person has any of these symptoms, they should seek medical help right away and immediately move to a cooler place, such as under shade or indoors. They should also take action to lower their body temperature with cool clothes, a cool bath or shower, and fans.
NHS 10 Year plan

The government has published its plan10-Year Plan which outlines a major transformation of the NHS, built around three core aims: moving care out of hospitals and into communities; replacing outdated systems with digital tools; and focusing on prevention rather than late intervention.
Central to the plan is the creation of Neighbourhood Health Services – integrated teams delivering everything from diagnostics to rehabilitation, mental health to lifestyle support, in local centres and on people’s doorsteps. Yet despite references to social care workers, the plan falls short of detailing how social care providers – the backbone of community support – will be empowered and resourced to lead this transformation.
Read More
Care England the representative body for independent adult social care providers, has welcomed the ambitions of the plan – but warns that without clarity on how adult social care is integrated into delivery, the plan risks being built on fragile foundations.
Professor Martin Green, chief executive of Care England, said: “This is a plan that talks our language – prevention, personalisation, community-based care. But we’ve heard similar before, and the challenge has always been implementation. The NHS cannot deliver this vision alone. If adult social care is not put at the centre of delivery – not just as a partner, but as a leader – this plan will falter.”
Care England emphasised that adult social care already provides much of the kind of support envisioned in the plan: long-term care for people with complex needs, step-down and reablement services, holistic community engagement, and workforce models rooted in local neighbourhoods.
Green added: “The plan speaks to a future we’ve already been building. But vision alone isn’t enough. Providers need clarity, investment, and status. Without a clear role for adult social care, this plan will leave a gap between policy and reality.”
The plan sets an ambitious target: by 2027, 95% of people with complex needs should have a co-produced personalised care plan – a major jump from the current 20%. Care England warns that without meaningful involvement of care providers – who know these individuals best – such targets will remain out of reach.
The timeline of the NHS plan also aligns with the forthcoming Casey Commission, expected to report next year.
Care England stresses that these two agendas – health reform and care reform – must move forward together.
Benefits you should receive.

Every year in the UK, £3.5 billion in benefits for pensioners goes unclaimed. Find out what you’re entitled to and how to claim it from the government.
Read More
Check out the website Lifeconnect24.co.uk excellent updates on entitlements.
Carers UK responds to IPPR paper

A new report published by the IPPR (Institute for Public Policy Research) highlights a rise in the number of people caring for 35 hours or more per week. Analysis for the report, conducted by the Joseph Rowntree Foundation, finds a significant increase. The number of people providing 35 hours or more a week of care has increased from 1.1 million in 2003/04 to 1.9 million in 2023/24 – an increase of over 70 per cent.
More Information
Emily Holzhausen CBE, Director of Policy and Public Affairs at Carers UK, said:
“Worryingly, we are seeing a growing number of people providing substantial care for disabled and older relatives from other data sets as well. In England and Wales, Census 2021 data shows a rise in the number of people providing 20-49 hours of care of 260,000 people (1.9% in 2021 compared with 1.5% in 2011) a slight rise in the proportion of people providing 50 or more hours of 152,000 people (2.8% in 2021 compared with 2.7% in 2011) and a deepening of the amount of care provided over time.
“This is significant because of the devastating impact that substantial unpaid care of over 20 hours per week can have on carers’ health, wellbeing and ability to juggle work and care. A growing number of carers are struggling with their own health due to the enormous pressures they are under.
“This is clearly a result of the shortage of adequate and properly funded social care and health services to support unpaid carers and the people they care for, in addition to an ageing population. Carers UK research shows that nearly two thirds of carers say they have no choice in providing care because there are no other care alternatives available. Without the support provided by unpaid carers our health and social care systems would quite simply collapse.
“We want the Government to commit to a funded, cross-government 10-year National Carers Strategy, delivering tangible progress and additional support for carers, their families, and those they care for – including robust investment in social care.”
A major clinical trial

A major clinical trial aiming to transform the diagnosis of Alzheimer’s disease
The ADAPT (Alzheimer’s Disease Diagnosis and Plasma p-Tau217) team, led by Professor Jonathan Schott and Dr Ashvini Keshavan at University College London (UCL), is evaluating whether a test measuring the protein p-tau217 in blood can help to diagnose Alzheimer’s disease earlier and more accurately than current methods.
Read More
The first ADAPT trial location began recruitment in Essex Partnership University NHS Foundation Trust on 28 August 2025 with 19 additional specialist NHS Centres planned across the UK.
The trial will examine whether providing the blood test results to patients and their clinicians near the start of an assessment for memory and thinking concerns is able to aid diagnosis and guide decisions on further investigations and treatments. The study will recruit participants through NHS memory services and will include people from diverse geographic, ethnic and economic backgrounds, and those living with other health conditions to ensure the findings are relevant and inclusive of the broader population.
Carer's living in cold.

Carers are much more likely than the rest of the UK population to be living in cold, unheated accommodation.
This is the stark finding of Running on Empty, a new report based on extensive analysis of datasets studying the income, wellbeing and expenditure of people across the UK. The research is also based on interviews with carers from across England, Scotland, and Wales.
The research was commissioned by Carers Trust and was carried out by Care Full.
Read More
Carers have always found it hard to make ends meet. Many have had to give up paid work altogether, or at least reduce their paid hours significantly, so they can care for a family member or friend. Many rely on benefits like Carer’s Allowance which fall short of what is needed for even a basic standard of living.
On top of these acute financial pressures, many carers find themselves more vulnerable to soaring household energy bills. That’s because, for many carers, reducing energy consumption is not an option. Carers need to keep houses warm and keep equipment running because this is essential for the person they are caring for
Government announce increase funding.

The government has announced increased funding to a scheme that will allow people to install adaptations such as stairlifts, ramps, accessible bathrooms and assistive technologies in their homes.
The government has recently announced that it will increase funding by £50 million this year for the Disabled Facilities Grant (DFG) which are provided by local councils to support older and Disabled people in making adaptations to their home.
These adaptations can range from small things like installing grab rails or lifting beds, sofas, or toilets to make standing up and sitting down easier, to larger infrastructure changes such as installing stair lifts, or widening doors for wheelchair access.
Read More
DFG funding supports around 60,000 people to make home adaptions each year, with an average grant of around £10,000, and this increase is expected to support an additional 5,000 people.
Calls have been made to reform the system with little change in the size of the average grant or the statutory upper limit of £30,000, since 2008.
Community services squeezed.

Community services are on the decline as local authorities try to square the circle of lower core funding, rising costs and higher demand.
As retired people spend significant amounts of time in their local communities, spaces like public libraries play a huge role in reducing isolation and providing access to services, while the provision of public toilets is vital for making town and city centres accessible.
Read More
But local authorities are in an almost impossible position when it comes to funding these services. Since the pandemic, during which overall funding from central government was temporarily increased, local authorities have been experiencing a triple burden on funding services. Core funding is lower in real terms while cost increases are higher than general inflation and there is also increased demand for services. This leaves local authorities with increasing gaps between the costs of providing services and the funding available.
Highest call volume on record

Alzheimer’s society busiest December on record.
The surge in calls is likely to be related to families spending more time together in recent weeks. Some people may have noticed, for the first time, changes in a loved one that could indicate dementia, while others faced increased care demands for someone already living with the condition.
Read More
Join Our Newsletter
Get the Latest news and advice
